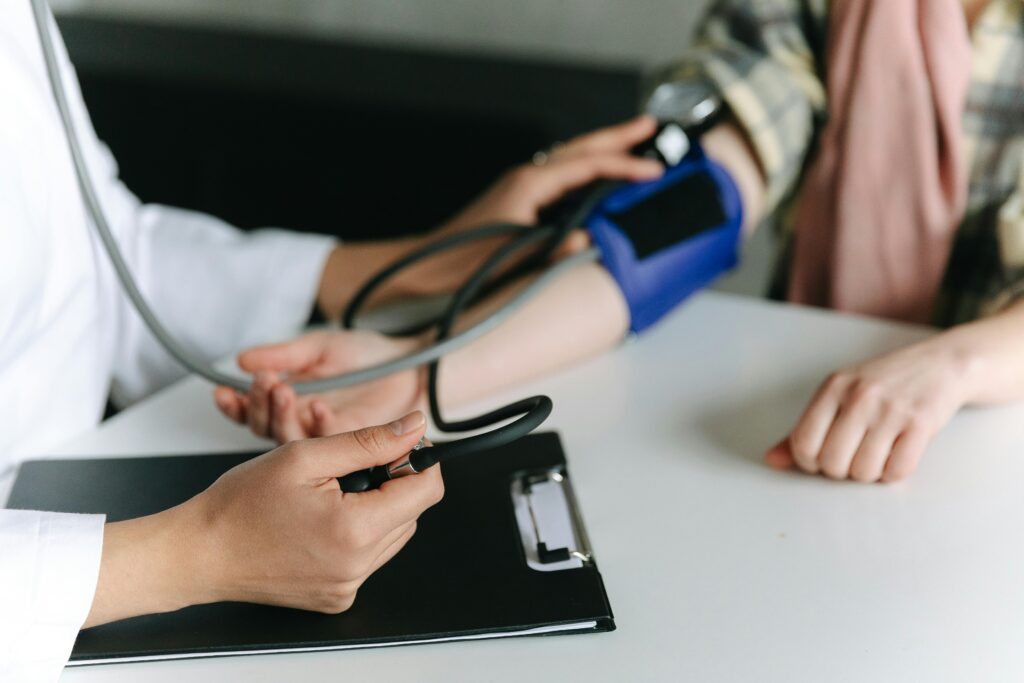
High blood pressure often goes undetected, but managing it doesn’t have to be a solo endeavor. Today’s approach to blood pressure care emphasizes collaboration—among yourself, your healthcare team, and even your daily routine—and values practical, sustainable choices.
First, embrace at-home monitoring as a key part of your care routine. A portable, clinically validated blood pressure monitor lets you track readings in the comfort of your own home—whether first thing in the morning before breakfast or in the evening after winding down. This avoids “white coat syndrome,” the temporary spike in blood pressure many people experience in medical settings that can skew in-office results. By logging these readings (note the date, time, and any relevant context, like a stressful day at work or a good night’s sleep) and sharing the record with your doctor, you turn vague worries into targeted, data-driven plans. This could mean adjusting medication dosages, switching to a different time of day for your pills, or refining small daily habits that impact your numbers.
Next, weave stress relief into your daily routine—no elaborate rituals required. For busy schedules, short, consistent practices work best: 10 minutes of mindful breathing before logging into work, a brisk 15-minute walk around the neighborhood during lunch, or even a few minutes of gentle stretching while waiting for coffee to brew. These small acts lower cortisol and adrenaline, the stress hormones that cause blood pressure to spike suddenly. Research from Harvard University supports this: consistent short-term relaxation practices, even just 20-30 minutes total per day, lead to steady, measurable improvements in blood pressure over weeks and months. It’s not about “eliminating stress” (an unrealistic goal for most) but about building small buffers that help your body regulate pressure more effectively.
Remember, your healthcare team is your greatest ally in blood pressure management—don’t hesitate to lean on them. Beyond your primary doctor, pharmacists can help you adjust medication schedules to fit your lifestyle (e.g., avoiding pills that make you drowsy during work hours) or clarify how to take medications correctly. Nurses often provide personalized lifestyle tips, from meal planning to safe exercise routines tailored to your fitness level. Even medical assistants can help you understand how to use your at-home monitor properly. Leveraging this full spectrum of support makes it far easier to stick to your care plan. This team-based approach isn’t just a trend; it aligns with modern clinical guidelines that prioritize personalized partnerships over one-size-fits-all solutions, recognizing that every person’s body and lifestyle is unique.
At the end of the day, small, consistent actions—paired with open, honest communication with your care team—are the foundation of long-term blood pressure control. It’s not about achieving perfection or overhauling your life overnight. It’s about building a sustainable system that works with your lifestyle: a 10-minute walk here, a logged blood pressure reading there, a quick chat with your pharmacist when you have questions. Over time, these small steps add up to big wins for your heart health and overall well-being. By viewing blood pressure management as a collaborative journey rather than a solo chore, you’ll find it easier to stay motivated and see lasting results.