Cardiovascular, cerebrovascular, and mental/pulmonary chronic diseases: A comprehensive analysis of the dangers of stroke, depressive disorders, and COPD.
Coronary Heart Disease (CHD)
Coronary heart disease (CHD) is short for coronary artery disease. CHD occurs because of atherosclerosis in the coronary arteries, the blood vessels that supply the heart with nutrients. These atherosclerotic plaques accumulate on the inner lining of the coronary arteries. The longer they accumulate, the more plaque builds up, severely narrowing or even blocking the lumen of the coronary arteries. This reduces blood flow to the myocardium, resulting in insufficient oxygen supply and impairing the heart's normal function. This leads to a series of ischemic symptoms, such as chest tightness, shortness of breath, angina, myocardial infarction, and even sudden death. Therefore, CHD is also called ischemic heart disease. CHD is a common and frequently occurring disease that seriously endangers human health. With the aging of my country's population and changes in lifestyle and dietary structure, the incidence of CHD has been increasing by 6.49% annually. Approximately 400,000 people in my country suffer myocardial infarction each year due to coronary atherosclerosis, making CHD one of the most serious diseases threatening human life and health. However, many people lack understanding of the dangers and severity of coronary heart disease. Due to differences in age, gender, physical condition, sensitivity, and disease progression among patients, the clinical manifestations of coronary heart disease vary greatly. Initially, patients may have no symptoms or discomfort. Occasionally, ischemic changes are discovered on an electrocardiogram during a physical examination, suggesting that the patient has "silent coronary heart disease" or "asymptomatic myocardial ischemia." In such cases, vigilance should be increased, regular check-ups should be conducted, and active prevention and treatment should begin.
Stroke
Stroke is the medical term for a sudden onset of cerebral circulatory disorders, also known as cerebrovascular accident. It refers to acute cerebral circulatory disorders caused by various triggering factors leading to narrowing, embolism, or rupture of cerebral arteries, resulting in symptoms and signs of temporary or permanent brain dysfunction. Stroke mainly includes ischemic stroke and hemorrhagic stroke. Strokes are broadly classified into ischemic and hemorrhagic types. Ischemic stroke, also known as cerebral infarction, is caused by vascular occlusion and accounts for 70%–80% of all strokes. Cerebral infarction accounts for 80% of sudden cerebrovascular deaths. A sudden cerebral infarction can be fatal or disabling, and most families consider it an unavoidable accident. However, experts believe that most cerebral infarction patients have underlying cerebral vascular stenosis. If this stenosis can be detected early through ultrasound or angiography and the vascular stenosis can be cleared in time, sudden cerebral infarction can be prevented. Clinical manifestations are mainly characterized by sudden loss of consciousness or sudden facial paralysis, hemiplegia, aphasia, and intellectual impairment. Only early recognition of stroke warning signs, timely diagnosis, and early treatment can effectively improve patient prognosis and reduce sequelae. The following factors can induce stroke:
1. Excessive blood pressure reduction: Lowering blood pressure too quickly or too much can easily cause insufficient blood supply to the brain, leading to cerebral infarction.
2. Excessive fatigue: Irregular lifestyle and excessive physical and mental exertion can easily cause blood pressure fluctuations, which is one of the factors leading to stroke.
3. Smoking and excessive alcohol consumption: Smoking aggravates cerebral arteriosclerosis and excites the autonomic nervous system; excessive alcohol consumption increases the burden on the heart, directly affecting the cardiovascular system and easily inducing stroke.
4. Sudden exposure to cold: Cold causes vasoconstriction, increases blood viscosity, and excites the sympathetic nervous system, easily inducing stroke.
5. High-fat diet and overeating: Both can lead to hyperlipidemia, aggravating arteriosclerosis and other metabolic diseases (obesity, diabetes, etc.), triggering stroke.
6. Anger: Anger can cause a sudden increase in blood pressure, inducing cardiovascular and cerebrovascular events.
7. Vomiting and diarrhea: Both can lead to dehydration, blood concentration, and increased blood viscosity, inducing cerebral infarction. Section 5 Depressive Disorders Depressive disorders are clinical syndromes or states centered on the subjective experience of depressed mood, caused by various factors. They include primary depressive disorders and secondary depressive disorders. Primary depressive disorder refers to a depressive syndrome excluding those caused by brain and physical illnesses, drug abuse, alcohol abuse, and other mental illnesses such as schizophrenia; its exact cause remains unknown. Secondary depressive disorder is a depressive syndrome caused by brain and physical illnesses, drug abuse, alcohol abuse, and other mental illnesses such as schizophrenia. Using Klerman's classification of depressive symptoms, it can be summarized as follows:
8. Affective symptoms: including sadness, anxiety, guilt, anger, hostility, and restlessness.
9. Behavioral symptoms: such as agitation, depressed appearance, psychomotor retardation, slow speech and thinking, crying, and suicidal behavior.
10. Attitudes towards self and environment: including self-blame, low self-esteem, helplessness, feelings of hopelessness and despair, and thoughts of death and suicide.
11. Cognitive impairment: including decreased thinking and attention.
12. Physiological changes and cognitive impairment (sometimes referred to as autonomic symptoms): such as inability to experience pleasure, loss of appetite, sleep disturbances, loss of energy, decreased interest, and physical discomfort.
Chronic Obstructive Pulmonary Disease
Chronic obstructive pulmonary disease (COPD) is a term used to describe emphysema, chronic bronchitis, or both, characterized by irreversible airflow limitation. Chronic bronchitis refers to chronic nonspecific inflammation of the trachea, bronchial mucosa, and surrounding tissues, characterized by recurrent episodes of cough, sputum production, and wheezing (lasting more than 3 months per year for 2 consecutive years). Obstructive emphysema is caused by harmful factors such as smoking, infection, and air pollution, leading to decreased elasticity, overinflation, and increased lung volume in the airways distal to the terminal bronchioles, accompanied by airway wall destruction, ultimately resulting in irreversible airway obstruction. Because most emphysema patients also have a history of chronic cough and sputum production, it is difficult to clearly distinguish between obstructive emphysema and chronic bronchitis. Therefore, chronic bronchitis and obstructive emphysema are collectively referred to as chronic obstructive pulmonary disease, or COPD for short. COPD often leads to pulmonary hypertension, cor pulmonale, and heart and lung failure, making it a common and serious health hazard. The characteristic symptoms of COPD are chronic and progressively worsening dyspnea, cough, and sputum production. Chronic cough and sputum production often precede airflow limitation by several years; however, some patients may not experience these symptoms. Common symptoms include:
① Dyspnea: This is the most important symptom of COPD and a major cause of physical weakness and anxiety. Patients often describe it as shortness of breath, wheezing, and difficulty breathing. Initially, it only occurs during exertion, gradually worsening until shortness of breath is felt even during daily activities and rest.
② Chronic cough: This is usually the first symptom. Initially, the cough is intermittent, worse in the morning, and later occurs in the morning and evening or throughout the day, but is less pronounced at night. A few cases do not produce sputum, and some cases have significant airflow limitation but no cough.
③ Sputum production: Coughing usually produces a small amount of mucoid sputum, which is more abundant in the morning for some patients. Sputum production increases with infection, often becoming purulent.
④ Wheezing and chest tightness: These are not specific symptoms of COPD. Some patients, especially those with severe COPD, experience significant wheezing, with widespread inspiratory or expiratory wheezing sounds on auscultation. Chest tightness often occurs after exertion and does not rule out a diagnosis of COPD, nor can the presence of these symptoms confirm a diagnosis of asthma.
⑤ Other symptoms: During the clinical course of COPD, especially in severe cases, systemic symptoms may occur, such as weight loss, decreased appetite, peripheral muscle atrophy and dysfunction, depression and/or anxiety, etc. Prolonged, severe coughing can lead to cough syncope, and hemoptysis may occur when complicated by infection.

Essential pre-exercise procedures for patients with hypertension: physical examination and safety assessment
This article emphasizes that hypertensive patients must consult a doctor and undergo a comprehensive physical examination and exercise stress test before starting exercise therapy to assess the risks of exercise. Scientific pre-examination can ensure safe and effective exercise, avoiding drastic fluctuations in blood pressure or triggering cardiovascular and cerebrovascular accidents due to inappropriate exercise.
2026-03-02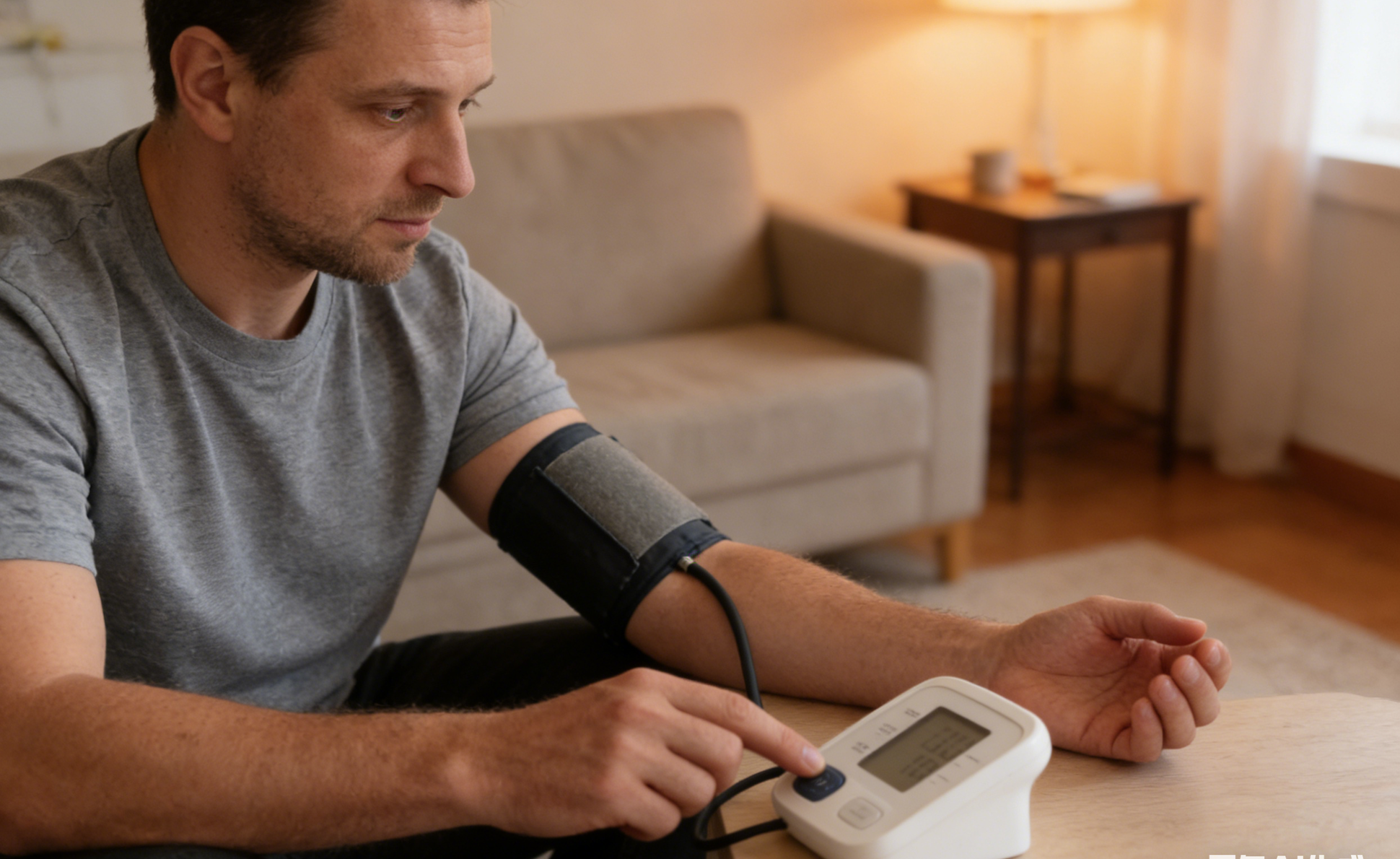
Exercise Safety Guidelines for Hypertensive Patients: Contraindications for Poor Condition and Excessive Running
This article reminds patients with hypertension to suspend exercise when they are in poor physical condition or fatigued, to avoid the risks of forced exercise. It also emphasizes that exercises such as running require strict control of intensity and duration; excessive exercise may be counterproductive. Scientific exercise is the only way to effectively help control and stabilize blood pressure levels.
2026-03-03
Why do people with hypertension need to have their blood pressure checked regularly? Importance and Frequency Guidelines
This article emphasizes the importance of regular blood pressure monitoring for patients with hypertension, explaining that irregular monitoring may delay diagnosis and increase the risk of cardiovascular, cerebrovascular, and renal complications. The article provides recommendations on blood pressure monitoring frequency for different disease conditions, aiming to help patients achieve more effective blood pressure control and management through regular monitoring.
2026-03-03