Analysis of the causes of postprandial hypotension and five prevention strategies
Why Does Postprandial Hypotension Occur?
1. After a meal, the body's digestive system allocates more blood to the body to more effectively digest and break down food and absorb nutrients. This significantly increases blood flow to the internal organs and relatively reduces blood flow to the peripheral vessels, leading to a decrease in venous return. Healthy individuals maintain normal postprandial blood pressure through mechanisms such as baroreflexes and neurohumoral factors. However, if one or more of these mechanisms malfunction, it can lead to insufficient compensation and postprandial hypotension.
2. Elderly individuals are more prone to postprandial hypotension due to decreased peripheral receptor sensitivity and reduced sympathetic nerve activity after meals.
3. Regarding dietary combinations, protein, fat, and carbohydrate intake can all contribute to postprandial hypotension, but carbohydrates empty from the stomach the fastest. Studies show that the greatest drop in postprandial blood pressure occurs after consuming carbohydrate-rich foods, with starch and glucose being the main contributing factors.
How to Prevent Postprandial Hypotension
1. First, everyone should understand the dangers of postprandial hypotension, especially 30-60 minutes after eating. Postprandial hypotension can lead to fainting and falls. 2. Discontinue unnecessary medications that may cause hypotension. If the patient has hypertension and needs to take antihypertensive drugs, avoid diuretics as much as possible. Additionally, antihypertensive medication can be taken between meals, and blood pressure should be monitored before and after meals.
3. Adjust lifestyle: Drink an appropriate amount of water (300-500mL) before meals; appropriately reduce the proportion of carbohydrates in food, especially avoiding high-sugar diets; eat smaller, more frequent meals to reduce the drop in blood pressure caused by insulin secretion stimulated by a sudden rise in blood sugar.
4. After meals, patients can engage in appropriate low-intensity activities, such as walking, to increase heart rate and cardiac output, but blood pressure should be monitored after exercise.
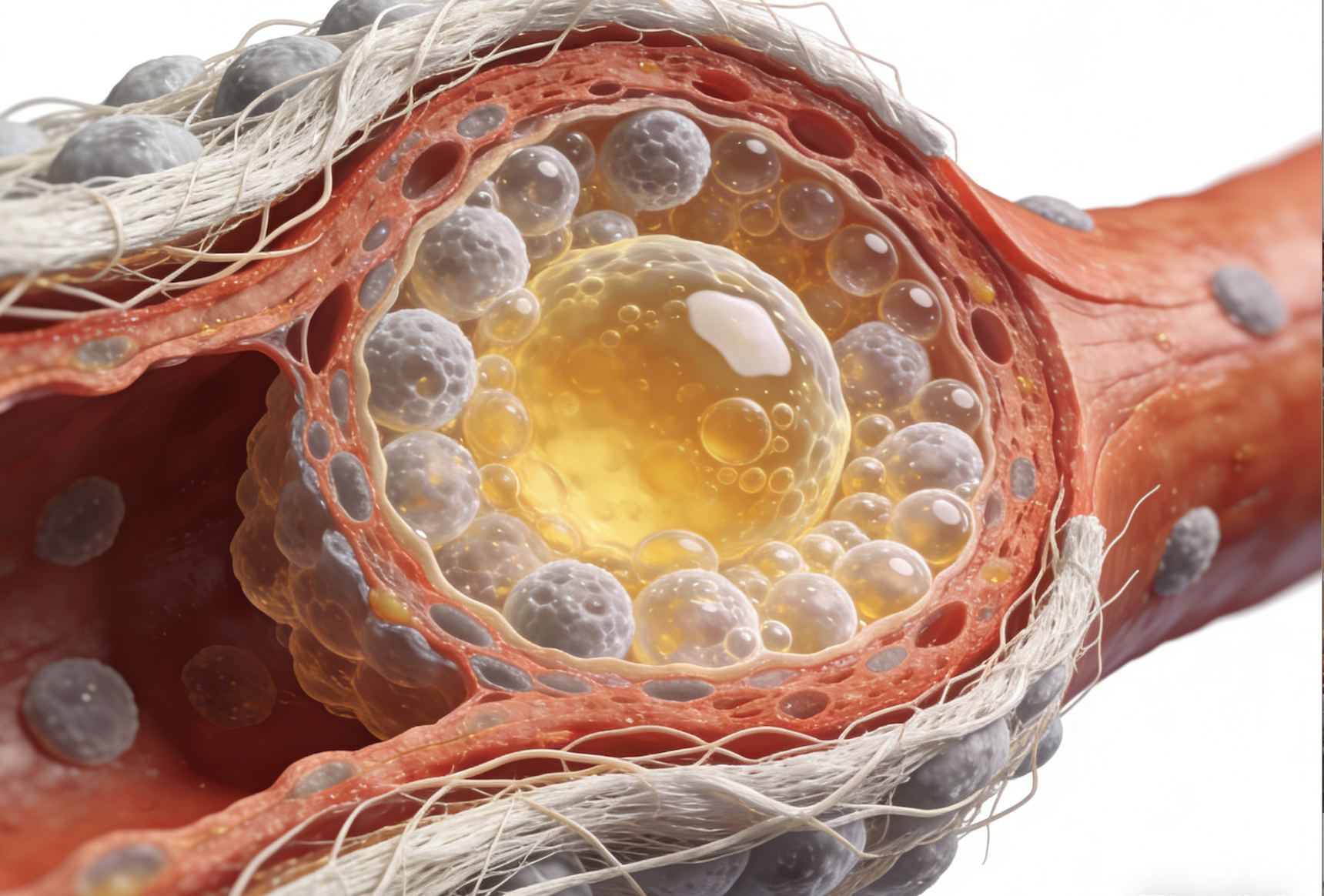
Analysis of common symptoms of hyperlipidemia: from silent onset to xanthoma manifestations
This article details the common symptoms and manifestations of hyperlipidemia (commonly known as high cholesterol), including its early, insidious nature and potential signs such as xanthomas. Understanding these symptoms helps in timely lipid testing, enabling early detection and management of lipid abnormalities.
2026-03-04
Analysis of Early Identification and Scientific Prevention Strategies for Hyperlipidemia
This article elucidates the importance of correctly understanding hyperlipidemia, revealing its hidden dangers of causing arteriosclerosis even when it is asymptomatic in its early stages. It emphasizes the necessity of lipid screening for high-risk groups and advocates for effective control of lipid levels through early intervention and scientific management.
2026-03-04
How to develop individualized lipid-lowering plans and reference standards for patients with hyperlipidemia
This article explains that the treatment of hyperlipidemia (i.e., hyperlipoproteinemia) requires an individualized lipid-lowering plan based on personal circumstances and provides specific reference values for blood lipid standards. Understanding these standards helps patients and doctors jointly set reasonable treatment goals and scientifically manage abnormal blood lipids.
2026-03-04