Detailed Explanation of the Five Major Complications of Hyperlipidemia and Their Pathological Connections
Fatty Liver: The liver is closely related to lipid metabolism, maintaining a dynamic balance in the processes of fat digestion, absorption, oxidation, transformation, and secretion. In patients with dyslipidemia, excessive nutrition leads to the accumulation of lipids within liver cells.
Thyroid hormones promote both the synthesis of cholesterol in the liver and the excretion of cholesterol and its metabolites from bile; therefore, thyroid hormones affect serum cholesterol production and degradation. In patients with hypothyroidism, lipid synthesis, mobilization, and degradation are all reduced, resulting in increased blood lipid concentrations. However, significantly elevated triglycerides are less common; the increase in lipoproteins is mainly due to elevated low-density lipoprotein (LDL) levels. Some researchers believe that patients with this disease have a defect in the LDL receptor pathway, and since LDL shows a significant negative correlation with thyroid hormone levels but a positive correlation with thyroid-stimulating hormone (TSH) levels, LDL can serve as an indicator of thyroid function.
Stroke: The risk of stroke and coronary heart disease in Asians is associated with elevated serum total cholesterol levels. However, this association is only observed between serum total cholesterol and ischemic stroke, and there is no correlation between total cholesterol levels and hemorrhagic stroke. Patients with hyperlipidemia have higher blood viscosity than normal individuals, making them more prone to thrombosis and stroke. Abnormal blood lipids can cause atherosclerosis, which is also a risk factor for stroke. Blood lipids can exist alone in the blood or combine with proteins to form lipoproteins; therefore, hyperlipidemia is also known as hyperlipoproteinemia. Decreased high-density lipoprotein (HDL) is also a contributing factor to cerebral infarction. Therefore, it is important not to unilaterally restrict fat intake, nor to overeat fatty and sweet foods; a scientifically and rationally planned diet is essential.
Hyperviscosity Syndrome: People often confuse hyperviscosity syndrome with hyperlipidemia. While both are important causes of cardiovascular and cerebrovascular diseases and often occur simultaneously, they are completely different conditions. Hyperviscosity syndrome is a pathological syndrome primarily characterized by increased blood viscosity. This condition increases blood flow resistance and slows blood flow, particularly affecting arterioles, capillaries, and microcirculation, leading to reduced tissue blood perfusion and causing headaches, dizziness, neck stiffness, and tinnitus. It can subsequently lead to dysfunction of organs such as the heart, brain, and kidneys. Patients should adopt comprehensive prevention and treatment measures, establishing a healthy lifestyle, adjusting their diet and eating habits, increasing water intake, maintaining a good mood, participating in appropriate exercise, and taking anti-viscosity medications to consolidate the therapeutic effect.
Nephrotic Syndrome: Patients with nephrotic syndrome often excrete large amounts of protein in their urine, resulting in decreased plasma protein levels. Hypoproteinemia can compensate by accelerating the synthesis of proteins, especially lipoproteins such as very low-density lipoprotein (VLDL), which can then be converted into low-density lipoprotein (LDL), possibly contributing to hyperlipidemia. Most patients with nephrotic syndrome have increased plasma lipids; even fasting plasma may appear milky. Although various lipids can be elevated, neutral lipids are increased the most, with cholesterol and triglycerides also increasing, and the degree of increase is negatively correlated with the decrease in plasma albumin. Prolonged hyperlipidemia in nephrotic syndrome can lead to atherosclerosis, thrombosis, and embolism. The incidence of vascular complications increases, therefore, hyperlipidemia requires careful treatment.
Pancreatitis: High serum triglyceride levels can cause acute pancreatitis. Many patients with hyperlipidemia experience intermittent upper abdominal pain, while their serum amylase levels are not diagnostic of pancreatitis; this may be an early sign of the condition. In some cases of acute and chronic pancreatitis, lipids are absorbed into the bloodstream after necrosis of adipose tissue in the greater omentum and peritoneum. The liver releases more triglycerides, and the activity of lipoprotein lipases, primarily from the pancreas, is reduced, hindering fat breakdown and resulting in hyperlipidemia. At this time, serum triglyceride and cholesterol concentrations are elevated, fasting serum appears milky and cloudy, and fundus examination reveals hyperlipidemic retinitis.

Detailed Explanation of the Correct Steps and Key Precautions for Measuring Blood Pressure
This article details the principles and key steps of blood pressure measurement using a cuff, including cuff selection, environmental preparation, patient positioning, and proper inflation and deflation techniques. Mastering these points ensures accurate and reliable blood pressure measurements each time, providing a valid basis for health monitoring.
2026-03-07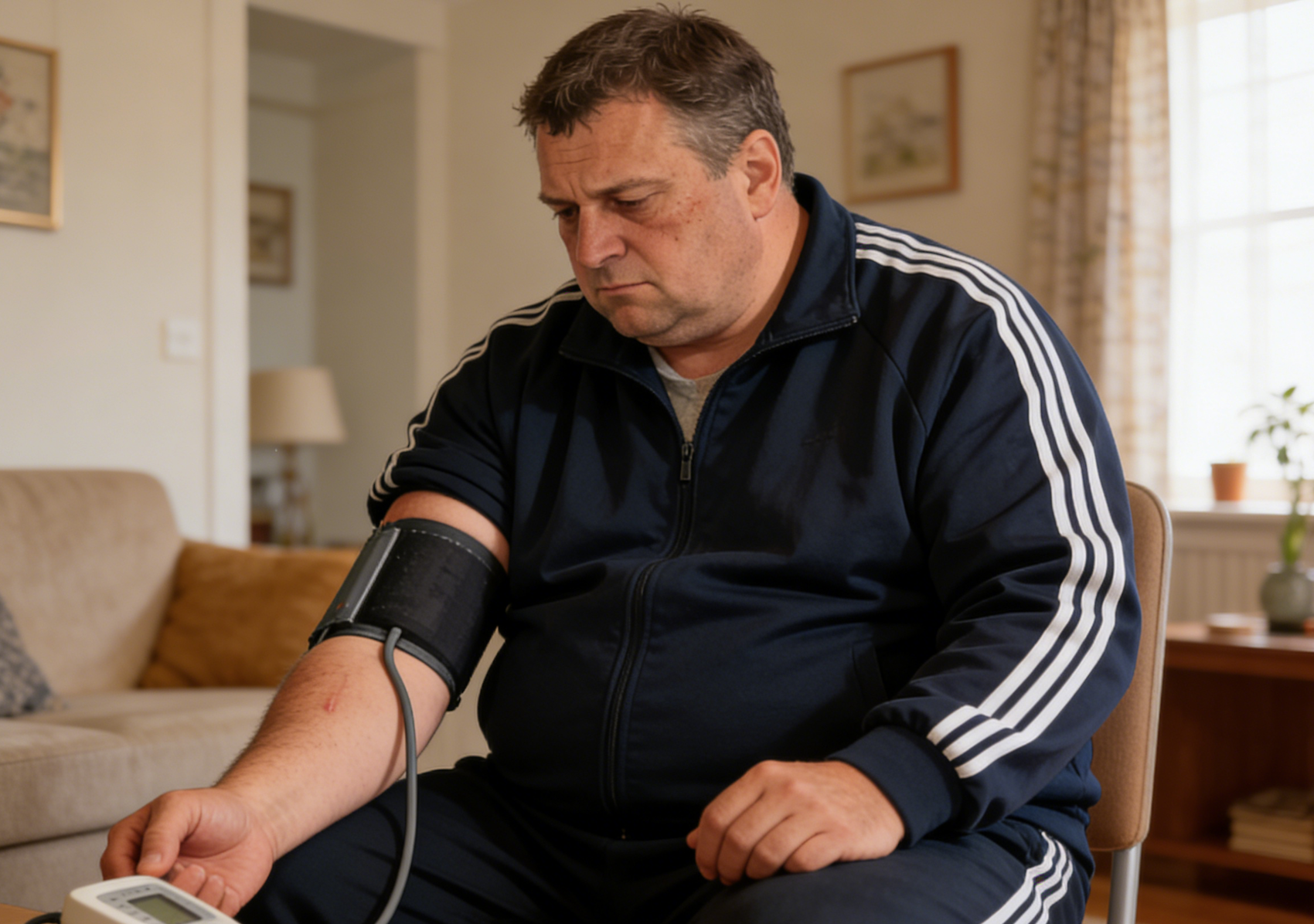
Detailed Explanation of the Definition of Hypertension and Analysis of its Seven Key Contributing Factors
This article elaborates on the definition of hypertension, clarifying the normal and elevated blood pressure ranges based on World Health Organization standards. It also systematically analyzes seven key contributing factors to elevated blood pressure, including genetics, obesity, smoking, and alcohol consumption, helping you comprehensively understand the causes of hypertension and effectively prevent it.
2026-03-07
Detailed Explanation of the Difference Between Hypertension and Hypertensive Disease and the Clinical Manifestations of the Four Major Types
This article clearly distinguishes between "hypertension" as a symptom and "hypertension as a disease" as an independent condition, and provides a detailed analysis of the characteristics and clinical manifestations of four types of hypertension: slow-onset, rapid-onset, etc. It helps you correctly understand the different natures of elevated blood pressure, the severity of different types of blood pressure problems, and provides a basis for timely diagnosis and treatment.
2026-03-08