The formation mechanism, classification, and systemic hazards of atherosclerosis
Atherosclerosis is a chronic inflammatory proliferative lesion of the arterial intima. Hypertension is closely related to atherosclerosis and is one of its main risk factors. Hypercholesterolemia (especially elevated LDL-C) easily leads to coronary heart disease and other atherosclerotic diseases. Its development includes lipid invasion, platelet activation, thrombosis, intimal damage, inflammatory response, oxidative stress, and activation of vascular smooth muscle cells. Because the lipids accumulated in the arterial intima appear as a yellow porridge, it is called atherosclerosis. Excessive low-density lipoprotein cholesterol (LDL-C) accumulates on the blood vessel wall, and long-term accumulation leads to endothelial cell damage. These low-density lipoproteins (LDL) are oxidized by free radicals, producing oxidized LDL. Oxidized LDL has high cytotoxicity. Monocytes and macrophages gather here, taking up large amounts of cholesterol, becoming foam cells. Cholesterol and damaged dead cells form visible clumps in the blood vessel wall, which are atherosclerotic plaques. The American College of Cardiology classifies it into 6 types based on pathological characteristics: Type I: Initial lesion. Small yellow spots appear on the intima, indicating foam cells. Type II: Lipid streaks. Type III: Pre-atherosclerotic plaque stage. Numerous lipid droplets appear extracellularly. Type IV: Atherosclerotic plaque. Lipids accumulate to form a lipid core. Type V: Fibrous plaque. Obvious connective tissue deposition forms a plaque cap on the surface of the lipid core. Type Va has a prominent lipid core and fibrous cap; Type Vb has obvious calcium salt deposition; Type Vc consists of collagen and smooth muscle cells. Type VI: Complex lesion. Fibrous plaques undergo hemorrhage, necrosis, ulceration, calcification, and mural thrombus formation. The dangers of atherosclerosis: First, due to thickening of the vessel wall and narrowing of the lumen, insufficient blood supply is caused by obstruction of blood flow; second, once an atherosclerotic plaque detaches, it easily leads to arterial blockage. Coronary atherosclerosis causes angina pectoris and myocardial infarction; cerebral atherosclerosis causes ischemic stroke and cerebral atrophy; renal artery atherosclerosis causes refractory hypertension; lower extremity atherosclerosis causes intermittent claudication or limb necrosis. The most dangerous situation is when cracks or ulcers appear on the surface of large plaques, leading to secondary thrombosis. It takes 10-15 years for an atherosclerotic plaque to mature from its initial formation. Coronary heart disease mostly occurs in people over 35 years old, with middle-aged and elderly people being more affected than young people, and men more frequently affected than women. In my country, more than one million people die each year from various types of coronary heart disease. Risk factors for coronary heart disease include: genetic factors, age (approximately doubling every 10 years after age 40), gender, diet, smoking, excessive alcohol consumption, psychological factors, hypertension, hyperlipidemia, obesity, and diabetes.

Detailed Explanation of Scientific Diagnostic Criteria for Secondary Prevention of Hypertension and Hyperlipidemia
This article details secondary prevention strategies for hypertension, emphasizing the importance of controlling blood pressure within the target range through standardized treatment and protecting target organs such as the heart, brain, and kidneys. It also provides an in-depth analysis of the composition of blood lipids and the diagnostic criteria for hyperlipidemia, helping patients understand how to scientifically manage their blood lipids and blood pressure to comprehensively prevent cardiovascular complications.
2026-03-06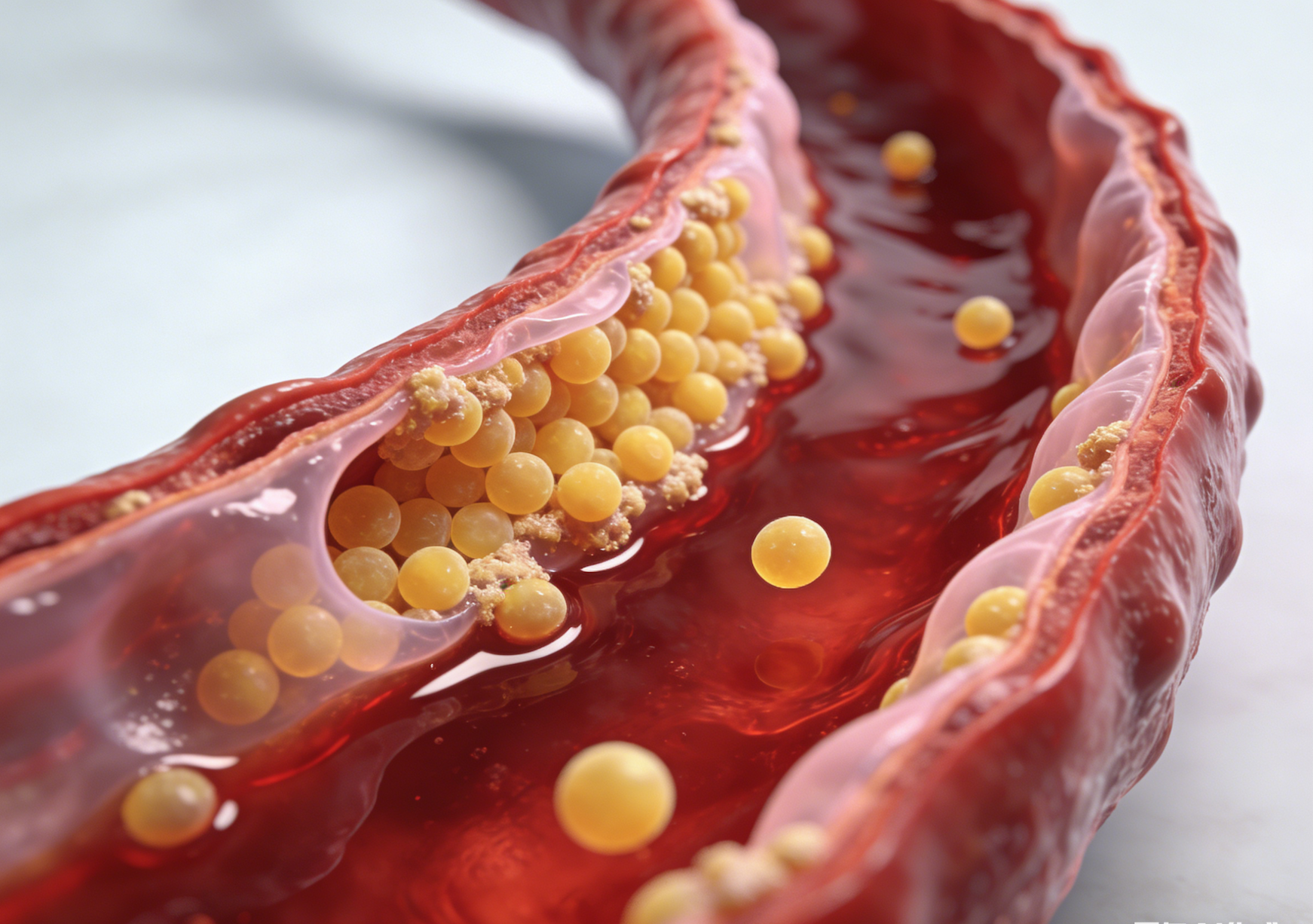
Analysis of diagnostic criteria, classification, and eleven high-risk groups for hyperlipidemia
This article details the diagnostic values for four key blood lipid indicators and analyzes four types of hyperlipidemia, including high cholesterol and high triglycerides. It also outlines eleven high-risk groups prone to hyperlipidemia, including those with a family history of the condition and those who are obese, to help you scientifically assess your own blood lipid health risks.
2026-03-09
The Dangers of Hyperlipidemia and its Three-Tier Prevention: A Comprehensive Analysis and Coping Strategies
This article details the serious harm that hyperlipidemia causes to multiple systems, including the heart, brain, and pancreas, emphasizing the importance of controlling blood lipids. It also systematically introduces the core measures for the three levels of prevention of hyperlipidemia, including drug therapy and lifestyle interventions, guiding patients to scientifically manage their blood lipid levels and prevent cardiovascular and cerebrovascular complications.
2026-03-09