Lifestyle interventions and blood glucose monitoring for diabetes: the cornerstone of personalized chronic disease management
Lifestyle interventions. Dietary therapy is the foundation of diabetes treatment and an indispensable component. Without dietary therapy, drug treatment will be ineffective. Estimate ideal weight (kg) = height (cm) - 105. Encourage daily weight measurement to encourage patients to pay attention and consciously control their weight to achieve the target. Ensure a varied diet with comprehensive and balanced nutrition, while keeping calories low. Calorie distribution: 25%-30% fat, 55%-65% carbohydrates, <15% protein. Limit salt intake to less than 6 grams/day, especially for hypertensive patients. Ensure calcium intake of 1000-1500 mg/day to reduce the risk of osteoporosis. Limit alcohol consumption, especially for obese patients, those with hypertension, and/or hypertriglyceridemia.
Exercise therapy.
1. Benefits of exercise: Strengthens cardiovascular function and improves overall health; increases insulin sensitivity; improves blood pressure and blood lipids.
2. Methods of exercise therapy. 3. Exercise Safety Issues. All diabetic patients should understand that exercise must be moderate. Excessive exercise has an adverse effect on blood sugar. Even moderate-intensity exercise carries the risk of inducing hypoglycemia. Insulin and insulin secretagogue dosages should be adjusted according to changes in blood sugar before and after exercise, and carbohydrate supplementation should be provided before and during exercise. High-intensity exercise can increase blood sugar levels during and after exercise, and may cause sustained hyperglycemia. In patients with type 1 diabetes or those with significantly elevated blood sugar before exercise, high-intensity exercise can also induce ketosis or ketoacidosis. Patients using insulin secretagogues or injecting insulin should begin exercising one hour after a meal.
4. Exercise Issues for Patients with Diabetic Complications. Patients with coronary heart disease have an increased risk of angina, myocardial infarction, or arrhythmia due to excessive exercise. Patients with proliferative retinopathy have an increased likelihood of lens hemorrhage. Patients with neuropathy have an increased risk of lower limb (especially foot) injuries and require special attention.
Blood Glucose Monitoring.
1. An important component of diabetes management. It can be used to reflect the effectiveness of diet control, exercise therapy, and drug therapy, and guide adjustments to the treatment plan. Blood glucose levels can be monitored through blood and urine tests, but blood glucose testing is ideal. The frequency of monitoring depends on the treatment method, treatment goals, disease condition, and individual financial situation. If possible, all patients should perform self-monitoring of blood glucose.
2. Precautions for self-monitoring blood glucose. When the condition is stable or has reached the control target, patients taking oral hypoglycemic agents can monitor blood glucose 1-2 times per week; patients injecting insulin should measure blood glucose at least 5 times a day in the initial stage, and 2-4 times a day after reaching the treatment goal; patients with type 1 diabetes should monitor blood glucose at least 3-4 times a day; during other acute illnesses or when blood glucose is >16.7 mmol/L (300 mg/dL), blood and urine ketones should be measured.
3. Timing and selection of blood glucose monitoring. Pre-meal blood glucose: Used when blood glucose is very high, or for those at risk of hypoglycemia (elderly, those with kidney damage); 2-hour postprandial blood glucose: Suitable for those whose fasting blood glucose is well controlled but still fails to reach the treatment target; Bedtime blood glucose: Suitable for patients injecting insulin, especially those using intermediate- or long-acting insulin; Nocturnal blood glucose: Used for those whose insulin therapy is close to the treatment target but whose fasting blood glucose is still high; when hypoglycemia symptoms occur; Patients with good or stable blood glucose control should monitor their blood glucose one or two days per week. Those with good and stable blood glucose control can monitor less frequently; Patients with poor/unstable blood glucose control or those with other acute illnesses should monitor their blood glucose daily until it is well controlled.
4. Glycated hemoglobin (HbA1c). HbA1c reflects the average blood glucose level over the preceding weeks and is the gold standard for evaluating blood glucose control regimens. The normal range is 4%–6%, and the target for diabetes control is <6.5%. If blood glucose control is not achieved or the treatment regimen is adjusted, HbA1c should be checked every 3 months. Once blood glucose control reaches the target, HbA1c should be checked at least twice a year.
5. Monitoring of urine glucose and ketones.
(1) Monitoring of urine glucose. Monitoring of urine glucose cannot replace monitoring of blood glucose; when urine glucose is negative, blood glucose monitoring should be used to understand changes in blood glucose; the target for urine glucose control should be negative.
(2) Monitoring of urine ketones. This is an important part of the daily diabetes management for patients with type 1 diabetes, diabetes mellitus complicated by pregnancy, and gestational diabetes. When considering blood glucose levels, the differences in measured values due to different measurement methods should be taken into account.

Detailed Guide to Personalized Lipid-Lowering Methods: From Diet and Exercise to Drug Therapy
This article emphasizes that lipid-lowering methods should be tailored to the individual, analyzing various options from dietary control and regular exercise to drug treatment (such as statins and fibrates) and lipid-lowering therapies. Regardless of the method, improving lifestyle, quitting smoking, and limiting alcohol consumption are crucial for regulating blood lipids, and an appropriate plan should be chosen based on individual blood lipid levels.
2026-03-11
A Comprehensive Explanation of Common Misconceptions about Hyperlipidemia and Scientific Prevention Strategies
This article systematically corrects common misconceptions such as "high blood lipids are nothing to worry about" and "no treatment is needed if there are no symptoms," emphasizing that blood lipids should be monitored regularly even without discomfort. It elaborates on medications to avoid, treatment of accompanying diseases, and a comprehensive management strategy combining diet, exercise, and lifelong medication to scientifically prevent and treat dyslipidemia.
2026-03-11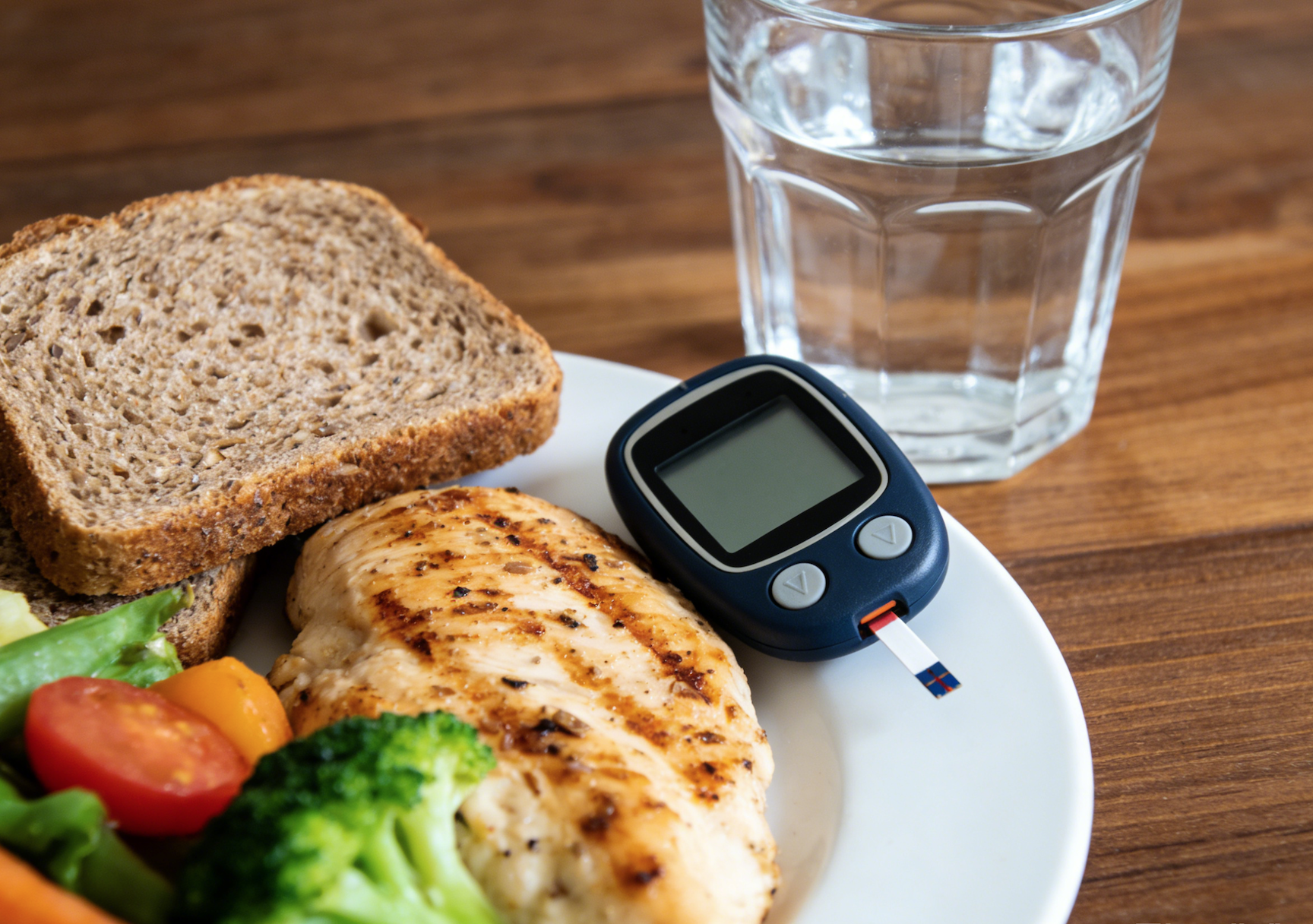
A Comprehensive Analysis of Common Misconceptions about High Cholesterol: Scientific Prevention and Correct Dietary Guidelines
This article provides an in-depth analysis of five common misconceptions about high blood lipids, including neglecting dietary adjustments and misunderstanding drug side effects, emphasizing the importance of comprehensive treatment for managing blood lipids. Properly controlling blood lipids requires a combination of a scientific diet and appropriate medication, avoiding extreme vegetarianism or excessively low cholesterol levels to maintain cardiovascular health.
2026-03-11