Post-coronary stent placement follow-up guidelines: a complete timeline from 1 month to 1 year post-procedure.
Post-Coronary Stent Implant Follow-up Schedule:
1 Month: One month after stent implantation, patients need to return to the hospital for a follow-up examination. This includes a complete blood count, coagulation function tests, biochemistry tests, and an electrocardiogram (ECG). Patients with myocardial infarction also need an echocardiogram.
Reason: After stent implantation, patients need to take antiplatelet drugs and statins. These medications affect the blood system and liver function. If the follow-up results are normal, the patient can continue taking the medication. If symptoms such as abnormal liver function occur, the doctor will need to determine whether the patient needs to change medication, reduce the dosage, or discontinue medication.
3 Months: Three months after stent implantation, even without any symptoms, patients should still return to the hospital for a follow-up examination. This includes a complete blood count, coagulation function tests, and biochemistry tests. If any symptoms occur, the doctor should determine whether a coronary CT angiography or CT scan is necessary.
Reason: The purpose of checking blood routine, coagulation function, and biochemistry is still to determine whether the medications the patient is taking have adverse effects on the patient's body. If there are no adverse effects, the patient can continue to take the medication long-term; if problems are found, symptomatic treatment should be given as soon as possible.
6 Months: Six months after stent implantation, the patient needs to go to the hospital for a follow-up examination. The examination includes blood routine, coagulation function, biochemistry, coronary CT or angiography. Patients with myocardial infarction need to undergo echocardiography.
Reason: Even if the patient has no symptoms, coronary CT or angiography is necessary to accurately determine whether there are any changes within the coronary artery stent. If stenosis or hyperplasia is found, it indicates that the patient has not controlled risk factors well or that medication treatment is insufficient, requiring early adjustment to prevent the stenosis from progressing severely.
1 Year: One year after stent implantation, the patient needs to go to the hospital for a follow-up examination. The examination includes blood routine, coagulation function, biochemistry, and echocardiography.
Reason: The patient has had a stent implanted for a full year, and the doctor needs to assess the patient's condition to determine if medication adjustments are necessary, such as discontinuing clopidogrel.
Cardiac stents are just one treatment option, and stent implantation surgery is a vascular reconstruction technique developed in the 20th century. It is now a very mature treatment method, and many county-level hospitals perform it very well. Therefore, patients do not need to worry about the technical aspects of stent surgery.
After stent surgery, patients must maintain an optimistic attitude. In addition to adhering to medication, they should engage in appropriate exercise such as walking or brisk walking, maintain a healthy diet, quit smoking and limit alcohol consumption, and have regular check-ups. Whether or not problems arise in the blood vessels after stent implantation depends not on the stent itself, but primarily on whether the patient manages their risk factors effectively.
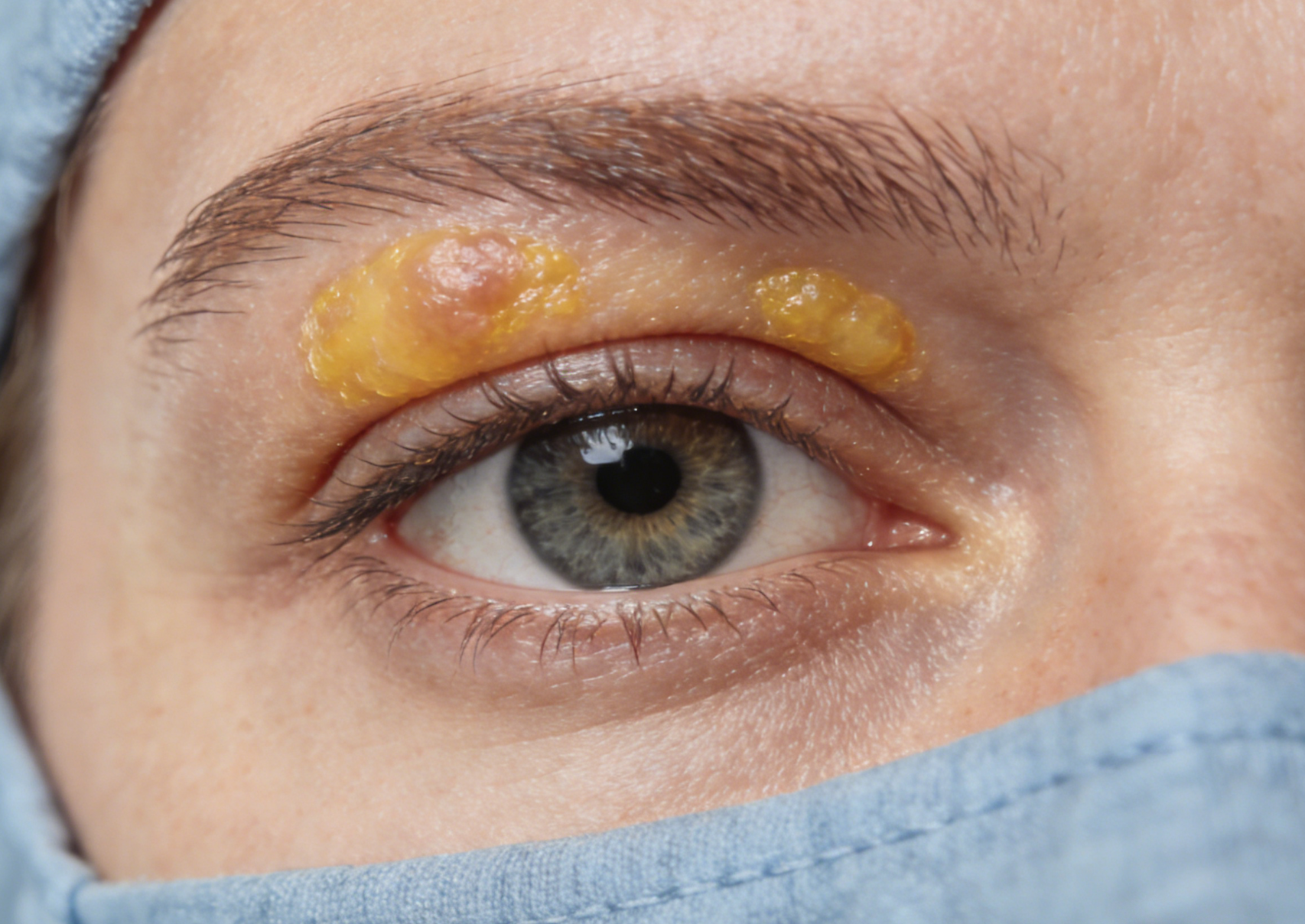
Analysis of Clinical Manifestations of Hyperlipidemia: Changes in the Eyes and Recognition of Skin Signals
This article details the clinical manifestations of high blood lipids in the eyes and skin, such as corneal arcus (arcus senilis) and fundus changes associated with hyperlipidemia. Understanding these symptoms helps in the early identification of potential lipid abnormalities. However, most cases of high blood lipids are asymptomatic, and regular monitoring of blood lipid levels is crucial for detecting problems.
2026-03-10
Detailed Explanation of Diagnostic Criteria for Hyperlipidemia: Six Subtypes and Clinical Manifestations
This article provides a detailed analysis of the six diagnostic subtypes of hyperlipidemia (hyperlipoproteinemia), from type I to type V, explaining the blood characteristics, cholesterol and triglyceride changes, and related diseases of each subtype. Understanding these subtypes helps in the accurate diagnosis of dyslipidemia and provides a basis for targeted treatment.
2026-03-10
A Comprehensive Analysis of Cholesterol: Good and Bad, Functions and Health Balance
This article provides a detailed analysis of the definition and classification of cholesterol, as well as its crucial role in key physiological functions such as bile synthesis, cell membrane construction, and hormone production. Understanding the dual role of cholesterol helps in the scientific management of blood lipid levels, maintaining a healthy lipid balance when necessary, and avoiding the risks of excessively high or low levels.
2026-03-10