Weight Loss Dietary Guide: Nutritional Principles and Staple Food Pairings for Individuals with High Blood Pressure, High Blood Sugar, and High Cholesterol
Summer Illness Prevention Rules for Diabetic Patients
In summer, diabetic patients should exercise outdoors in the morning or evening, and indoors if exercising at midday. When exercising indoors, it's best to turn off the air conditioner or avoid setting the temperature too low to prevent catching a cold after exercise. After outdoor exercise, do not immediately enter an air-conditioned room; change clothes promptly and avoid taking a cold shower.
During summer exercise, sweating is more pronounced, so it's important to know when to replenish fluids: Adequate hydration during exercise increases plasma volume, reduces blood flow resistance, and improves cardiac efficiency and exercise duration. Replenish fluids more readily 30 minutes after exercise. Note that the correct method is to drink small amounts frequently, no more than 100mL at a time, preferably warm water, and avoid ice water.
In summer, the body's insulin sensitivity increases, which is beneficial for lowering blood sugar levels. Increased activity levels and hot weather in summer also accelerate metabolism and energy expenditure, further contributing to lower blood sugar levels. These two factors are the main reasons for lower blood sugar levels in summer, making it the optimal time for diabetic patients to receive treatment.
Summer Health Preservation for Diabetic Patients: Nourishing Yin and Strengthening Qi is Key
It's worth noting that summer treatment for diabetes should also focus on "nourishing Yin and strengthening Qi," applying traditional Chinese medicine methods to strengthen the spleen, consolidate sweat, nourish Yin, and enhance physical strength. Additionally, taking Qi-tonifying herbs can improve the body's sensitivity to insulin, helping to maintain normal blood sugar levels.
Some may think that since blood sugar is lower in summer, can the dosage of medication be reduced? Diabetic patients must remember that they should never arbitrarily stop or reduce their medication; on the contrary, blood sugar is easier to control in summer, so treatment should be strengthened, and sometimes the dosage can even be slightly increased to bring blood sugar down to normal. After blood sugar levels have returned to normal and remained stable for a period of time, medication reduction can be considered under the guidance of a doctor.
Three Important Precautions for Diabetic Patients in Autumn
Precaution 1: Prevent Autumn Dryness and Replenish Water Promptly. Don't wait until you're thirsty to drink water. In early autumn, the "autumn tiger" (a period of hot, dry weather) is rampant, and the body consumes a lot of energy. Everyone should pay attention to replenishing water during this season, and this is especially important for diabetic patients. Diabetic patients sweat a lot, and the diuretic effect of high blood sugar makes them more prone to dehydration. Insufficient hydration can easily lead to blood clots and kidney dysfunction. Diabetic patients should drink plenty of plain water, fruit and vegetable juices, soups, and weak tea. They can also drink some homemade herbal teas to replenish lost fluids. Diabetic patients can drink Ophiopogon japonicus infusion daily, which can replenish fluids and nourish yin.
Secondly, according to the traditional Chinese medicine principle of "moistening dryness," the autumn diet for diabetic patients should focus on sweet, bland, and moisturizing foods. Fruits and vegetables such as radishes, cucumbers, winter melons, cauliflower, and cabbage are best cooked by stewing, cold salads, stir-frying, boiling, or steaming. Daily intake of high-quality protein, such as meat, dairy products, and soy products, is essential. For diabetic patients who sweat a lot in hot weather or participate in outdoor activities, daily salt intake should be increased slightly, from 5-6g to 6-7g, or they can supplement their diet with seafood such as kelp and dried shrimp to replenish salt. However, patients with high blood pressure, kidney disease, or edema should eat less salt, as it can worsen edema.
Precaution 3: Pay attention to food hygiene and prevent gastroenteritis. Summer and autumn are high-incidence seasons for intestinal diseases. Diabetic patients have weaker resistance, so they should pay special attention to food hygiene to prevent diarrhea. Diabetic patients should try to avoid raw and cold foods, because on the one hand, raw and cold foods are prone to spoilage, and on the other hand, in hot weather, the human body is prone to spleen and stomach imbalances. Raw and cold foods can easily induce gastrointestinal discomfort, causing acute gastroenteritis, vomiting, or diarrhea, leading to dehydration and electrolyte imbalance, inducing hyperosmolar coma, and possibly inducing hypoglycemia due to reduced carbohydrate absorption.
Diabetic Patient Winter Disease Prevention Rules: In winter, the temperature is low, and people change their diet accordingly to keep warm, with more greasy and rich foods on the table. In addition, the weather is cold and outdoor activities are significantly reduced, which can easily lead to elevated blood sugar. The cold winter temperatures can stimulate the sympathetic nervous system, increasing the secretion of catecholamines, which can easily lead to elevated blood sugar, platelet aggregation and thrombus formation, high blood pressure, and coronary artery spasm, thus worsening coronary heart disease symptoms and triggering angina.
Furthermore, many patients do not have a blood glucose meter at home, and the cold weather and reluctance to go to the hospital to check their blood sugar are also contributing factors to the increased risk of elevated blood sugar in winter. Understanding these factors necessitates that patients monitor their blood sugar more frequently in winter and make timely adjustments to their diet and medication. Experts advise that patients with mild diabetes should have their blood sugar checked at least once every two weeks in winter, or monitor it themselves. Patients with severe diabetes are more prone to complications due to sudden spikes in blood sugar in winter and should ideally monitor their blood sugar daily, keep detailed records, and promptly inform their doctor of any changes to prevent elevated blood sugar levels in winter.
How can diabetic patients prevent osteoporosis in winter? Diabetic patients are highly susceptible to osteoporosis, a serious condition that causes widespread pain, restricts movement, and can even lead to fractures, severely impacting their quality of life. Regular sun exposure is a crucial measure for preventing osteoporosis. In the cold winter, the warm sunlight acts like a natural stimulant. Ultraviolet rays in sunlight trigger a series of physiological changes beneficial to diabetic patients, promoting blood circulation and metabolism, and enhancing the body's absorption of calcium and phosphorus. Sun exposure also helps the body produce vitamin D, promoting bone calcification and growth. Furthermore, the ultraviolet rays in sunlight have strong bactericidal properties, reducing the chances of various viral and bacterial infections.
However, more sun exposure is not necessarily better; excessive sun exposure can induce skin diseases. Therefore, it is essential to choose an appropriate time for sun exposure based on one's own physical condition. Generally, the "golden hours" are before 10 am and after 3 pm, aiming for 30-60 minutes of sun exposure daily. Elderly diabetic patients should begin sunbathing half an hour after sunrise, as the air is humid and the sunlight is warm and gentle at this time.

Analysis of Special Treatments for Hyperlipidemia: From Stroke Prevention to Diabetes Management
This article details the unique roles of lipid-lowering therapy in preventing stroke, improving kidney disease and fatty liver, and provides treatment guidance for patients with dyslipidemia who also have hypertension, postmenopausal women, and diabetes. This content is of significant reference value for comprehensive lipid management and optimizing treatment strategies.
2026-03-03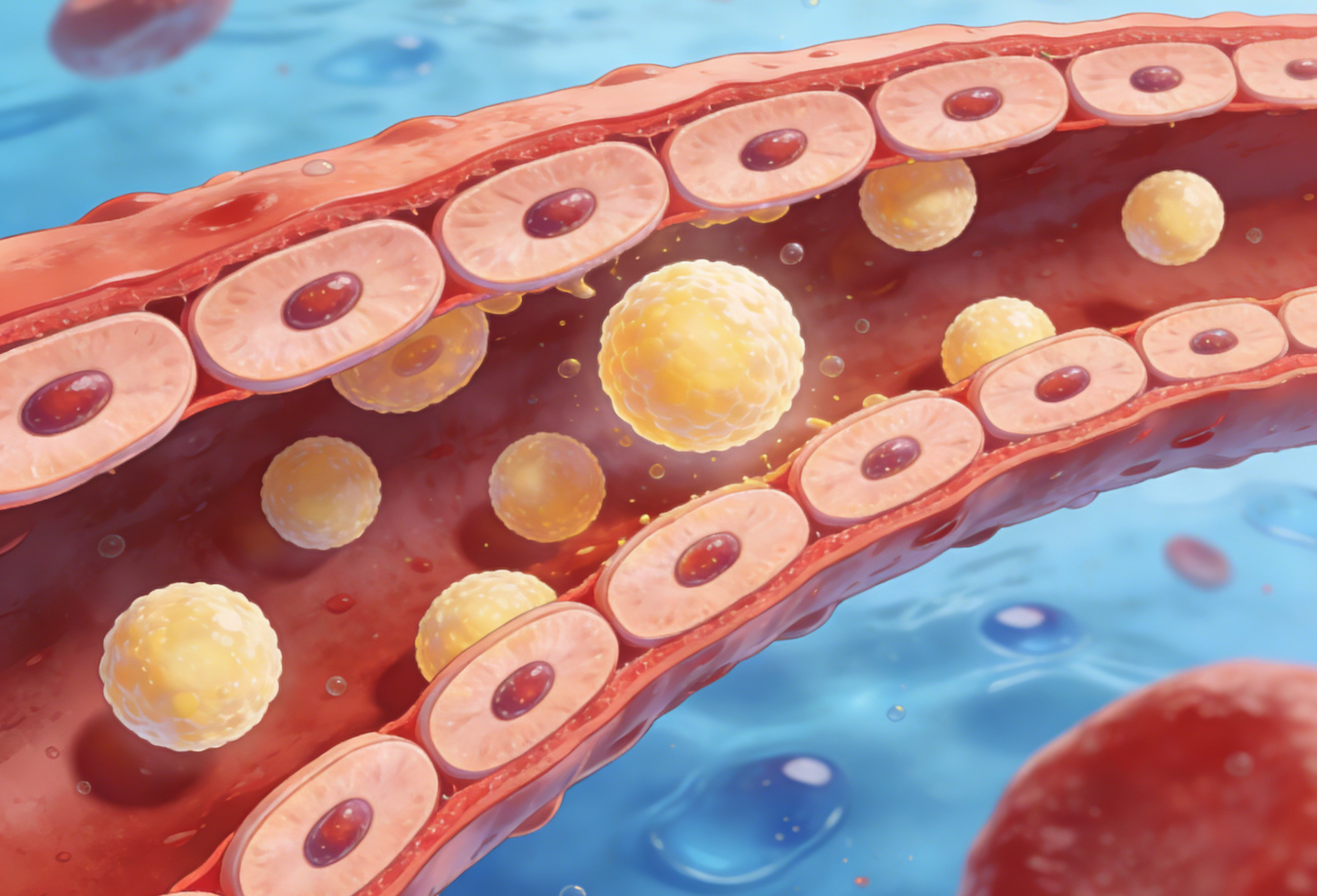
Analysis of the mechanisms of hyperlipidemia: Influence of endogenous and exogenous factors and age
This article details the internal and external causes of hyperlipidemia, elucidates the metabolic mechanisms of cholesterol and triglycerides, and explains how factors such as age, diet, and disease affect blood lipid levels. Understanding these factors helps manage abnormal blood lipids at their source and effectively regulate blood lipid fluctuations.
2026-03-03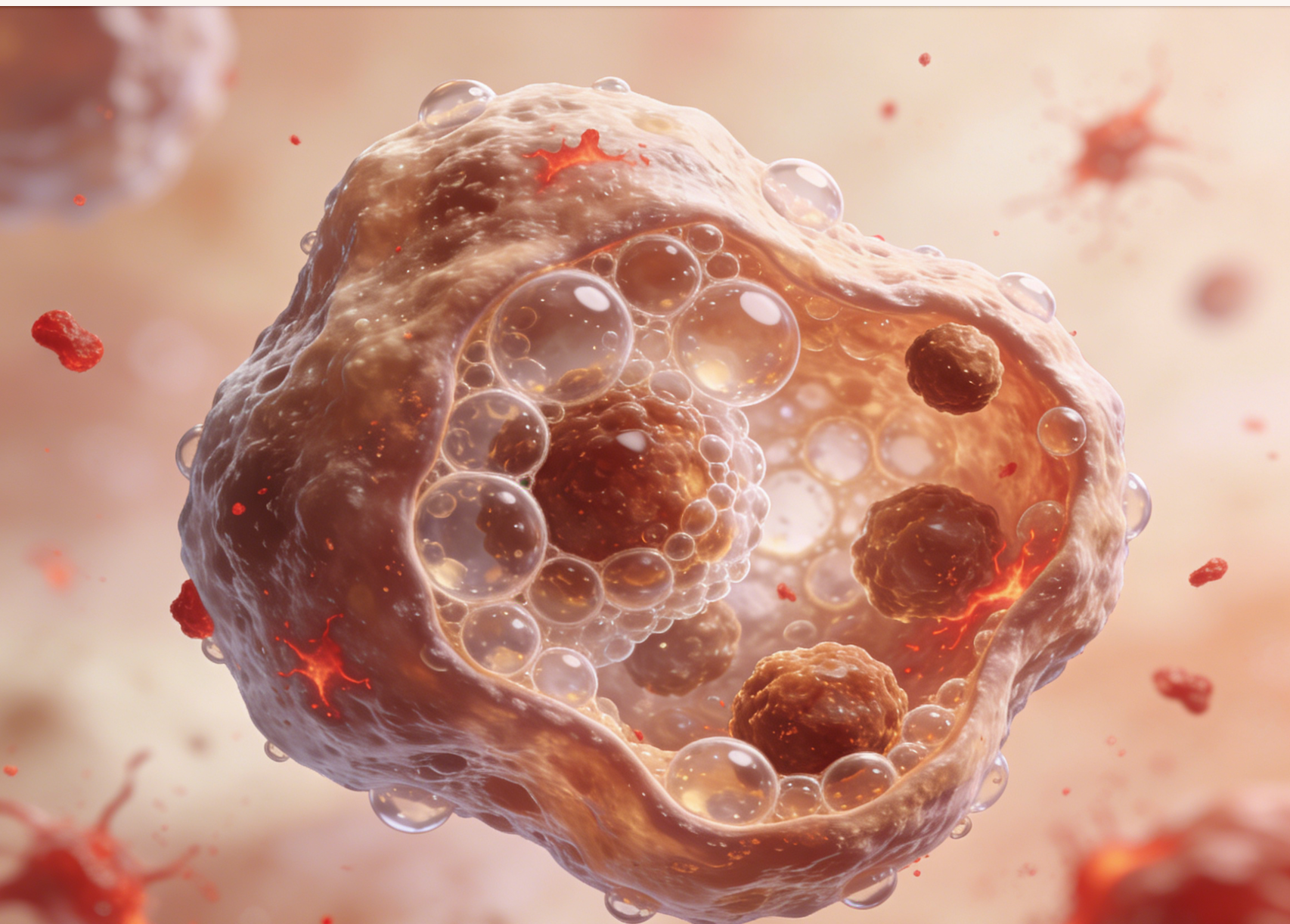
Detailed Explanation of the Pathogenesis of Hyperlipidemia: Diagnostic Criteria, Etiology, and Classification
This article details the diagnostic criteria, pathogenesis, and main classifications of hyperlipidemia, and elucidates the causes of primary and secondary hyperlipidemia, including genetic, dietary, and related disease factors. Understanding these factors helps in recognizing the root causes of dyslipidemia, thereby enabling more effective management of blood lipid levels.
2026-03-03